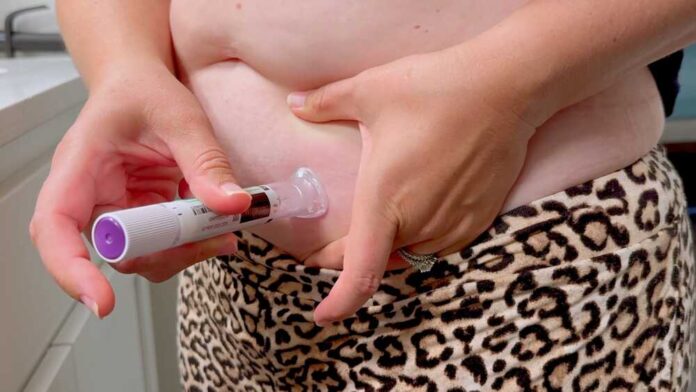
The increasing prescription rate of Glucagon-like peptide 1 (GLP-1) receptor agonist medications, such as Ozempic and Wegovy, for chronic weight management in the United States has focused attention on issues of equitable access within the national response to the ongoing obesity crisis. These drugs, originally developed for diabetes, have been approved by the Food and Drug Administration (FDA) for weight loss, marking a notable evolution in medical treatment. However, significant financial and regional barriers are currently limiting their availability to many Americans.
Story Highlights
- GLP-1 receptor agonist drugs have become a core component of medical obesity treatment.
- Access to these medications is reportedly uneven, with high-demand “hot spots” emerging across the country.
- High costs and varying insurance coverage present a primary financial barrier for patients seeking long-term adherence.
- The situation raises concerns regarding the potential for these new treatments to increase existing societal health disparities.
GLP-1 Medications and Their Use in Chronic Weight Management
GLP-1 receptor agonists, which include medications such as Ozempic, Wegovy, and Mounjaro, are now widely prescribed for weight loss following clinical trials that demonstrated their effectiveness. The FDA’s approval of these drugs for chronic weight management represents a fundamental change in the medical approach to obesity.
The rise in demand for these pharmaceuticals has, in some areas, exceeded current supply, leading to reports of heightened competition for access in certain regions of the country, described as “hot spots.” This imbalance in availability has fueled discussion regarding the equitable distribution and affordability of the medications.
America’s obesity crisis meets the Ozempic boom as data reveals GLP-1 hot spots https://t.co/D1RSrK2X5N #usa #feedly
— Music World 360 (@MusicWorld360x) November 9, 2025
Economic and Coverage Barriers to Access
A key challenge for many individuals seeking GLP-1 therapies is the substantial financial cost. Despite the demonstrated benefits, the medications often have high retail prices and are not consistently covered by all insurance plans. This can result in significant out-of-pocket expenses for patients, potentially hindering the long-term use necessary for effective treatment and contributing to wider health disparities. This issue is particularly relevant as obesity is statistically more prevalent in lower-income communities, which often face the greatest difficulty in affording new and expensive treatments without robust financial support.
Healthcare professionals are navigating the challenge of advocating for patient access to these treatments while managing the practical limitations imposed by health insurance coverage. The scenario underscores a potential need for policy discussions aimed at balancing cost management with ensuring patient access to effective obesity pharmacotherapy, irrespective of socioeconomic status.
Weight-loss drugs are booming in these US states — with nearly 25% on GLP-1 meds in one obesity hot spot https://t.co/71QJ5pLjgM pic.twitter.com/Zqvcd9bWrW
— New York Post (@nypost) November 9, 2025
Long-Term Considerations and Research
While GLP-1 drugs represent an advancement in obesity management, ongoing studies are focused on their long-term safety profiles and effectiveness.The data suggesting these medications may reduce cardiovascular and metabolic risks is viewed as positive, but their role in addressing the complex, underlying causes of obesity is acknowledged as partial.
As the healthcare sector adapts to these new treatments, continued research is essential for understanding the widespread implications of GLP-1 use. Legislative and industry leaders are tasked with developing solutions that ensure medical innovations contribute to reducing, rather than worsening, existing inequities in public health.
Sources:
- America’s obesity crisis meets the Ozempic boom as data reveals GLP-1 hot spots
- Weight-loss pills replacing GLP-1 shots will be ready by March, Dr. Oz tells FOX Business
- Weigh Loss drugs are boominng